What Is Cortisol Face? Symptoms in Women You Shouldn’t Ignore
I remember the morning I stood in front of my bathroom mirror, pressing two fingers into my cheek and watching the puffiness slowly spring back. My skin looked inflamed. There was a new cluster of breakouts along my jawline that hadn’t been there the week before. I’d been sleeping seven hours a night, eating reasonably well. So why did I look like I hadn’t slept in three days?
It wasn’t until I started digging into the connection between cortisol face symptoms in women that everything made sense. The puffiness, the breakouts, the dullness, the under-eye hollows that no concealer could fix. It was all my stress hormones talking. And if you’ve landed on this page, there’s a good chance your skin is trying to tell you something too.
Cortisol face is real. It’s not just a TikTok buzzword. It’s a genuine physiological response to chronic stress, one that shows up on your face before it shows up anywhere else. In this guide, I’m breaking down exactly what it is, what it looks like, what’s actually happening inside your body, and how to start reversing it naturally.
What Is Cortisol Face? The Science in Plain English
Cortisol is your body’s primary stress hormone, produced by the adrenal glands sitting just above your kidneys. In short bursts, it’s genuinely useful. It sharpens your focus, gives you a burst of energy, and helps you respond to a crisis. The problem starts when it never switches off.
When you’re under chronic stress (the kind that drags on for weeks, months, or years) your cortisol levels stay persistently elevated. According to research published by the National Institutes of Health, prolonged cortisol elevation disrupts nearly every system in your body, including the ones responsible for keeping your skin healthy, firm, and clear.
Here’s what excess cortisol does to your face specifically:
- Breaks down collagen and elastin: the structural proteins that keep skin plump and firm
- Triggers systemic inflammation: which manifests as puffiness, redness, and flare-ups
- Disrupts the skin barrier: leading to dehydration, sensitivity, and dullness
- Spikes oil production: which clogs pores and causes hormonal acne, especially along the jawline
- Causes fluid retention: particularly in the face, creating that characteristic puffy, swollen look
The term became popular on social media when people started recognising patterns in their own skin. A rounder, puffier face, persistent acne, and an overall tired look that didn’t improve no matter what products they used. What they were seeing was their cortisol levels, written on their face.
Cortisol Face Symptoms in Women: What to Look For
This is where I want to be specific, because most articles online give you a vague list that could describe literally any bad skin day. Cortisol face symptoms in women have a distinct pattern. They tend to appear together, they worsen during high-stress periods, and they don’t respond well to topical fixes alone.
1. Facial Puffiness, Especially in the Morning
This is the most recognisable sign. You wake up, look in the mirror, and your face looks rounder and more swollen than it did the night before. It’s not weight gain. It’s fluid retention driven by elevated cortisol. High cortisol triggers your body to hold onto sodium and water, and your face absorbs the most visible evidence of that.
The puffiness is typically worse around the cheeks, under the eyes, and along the jawline. It usually improves slightly by afternoon, which is one clue that it’s cortisol-related rather than structural.
2. Jawline and Chin Acne That Won’t Quit
Hormonal acne along the lower face, the jawline, chin, and sometimes the neck, is one of the clearest cortisol face symptoms in women. Here’s why: cortisol triggers a surge in androgens (male hormones that both men and women produce), which signals sebaceous glands to produce more oil. That excess oil, combined with a compromised skin barrier, creates the perfect environment for cystic, painful breakouts.
What separates cortisol acne from regular breakouts is timing. They tend to appear or worsen during or just after stressful periods. A hard week at work, an emotionally draining situation, a stretch of poor sleep. They’re often deep, inflamed, and slow to heal.
3. Dull, Tired-Looking Skin That Products Can’t Fix
Collagen is what gives your skin that bouncy, lit-from-within quality. Cortisol actively degrades collagen over time, according to a review in Clinics in Dermatology. When collagen breaks down faster than your body can replace it, skin loses luminosity. It starts to look flat, grey, and tired, even when you’re technically rested.
No serum fixes this on its own, because the problem isn’t topical. The dullness is coming from inside, from an ongoing breakdown process that skincare can only partially compensate for.
4. Fine Lines Appearing Faster Than They Should
I’ve spoken to women in their late twenties who are convinced they’re ageing prematurely. In many cases, they’re right, but not because of genetics. Chronic cortisol exposure accelerates skin ageing by depleting collagen and impairing skin cell turnover. Lines around the eyes and mouth deepen. Forehead lines become more pronounced. The skin loses the subtle thickness that makes it look youthful.
This is one of the most underreported cortisol face symptoms in women, because it’s easy to chalk up to getting older rather than recognising it as a sign of a hormonal imbalance.
5. Under-Eye Darkness and Hollowing
The under-eye area is particularly sensitive to cortisol fluctuations. Elevated cortisol disrupts your sleep architecture, specifically your deep sleep cycles, which is when your skin does its repair and regeneration work. Poor sleep quality (even if the hours look fine on paper) results in blood pooling under the thin skin beneath the eyes, reduced circulation, and that sunken, hollow appearance that makes you look perpetually exhausted.
6. Redness, Flushing, and Skin Sensitivity
Cortisol is pro-inflammatory at chronically high levels. This can trigger or worsen conditions like rosacea, eczema, and general skin sensitivity. Women who never had reactive skin suddenly find that their face flushes easily, reacts to products it previously tolerated, or stays persistently red across the cheeks and nose.
7. Thinning Skin That Bruises Easily
This is a less commonly discussed symptom but an important one. According to the Cleveland Clinic, chronically elevated cortisol thins the skin over time by inhibiting the fibroblasts responsible for producing new collagen and elastin. Thin skin bruises more easily, wrinkles more readily, and heals more slowly.
Cortisol Face vs Moon Face: What Is the Difference?
These two terms are often used interchangeably online, and that’s a problem, because they have meaningfully different causes and different implications for your health.
Cortisol face refers to the visible skin changes caused by chronically elevated cortisol from lifestyle stress: ongoing work pressure, emotional stress, poor sleep, blood sugar dysregulation. It’s common, it’s reversible, and it responds to lifestyle changes.
Moon face is a specific medical term describing the rounded, swollen facial appearance associated with Cushing’s syndrome: a condition caused by extremely high cortisol levels, either from a cortisol-secreting tumour or from long-term use of corticosteroid medications.
Here’s a side-by-side breakdown to help you tell them apart:
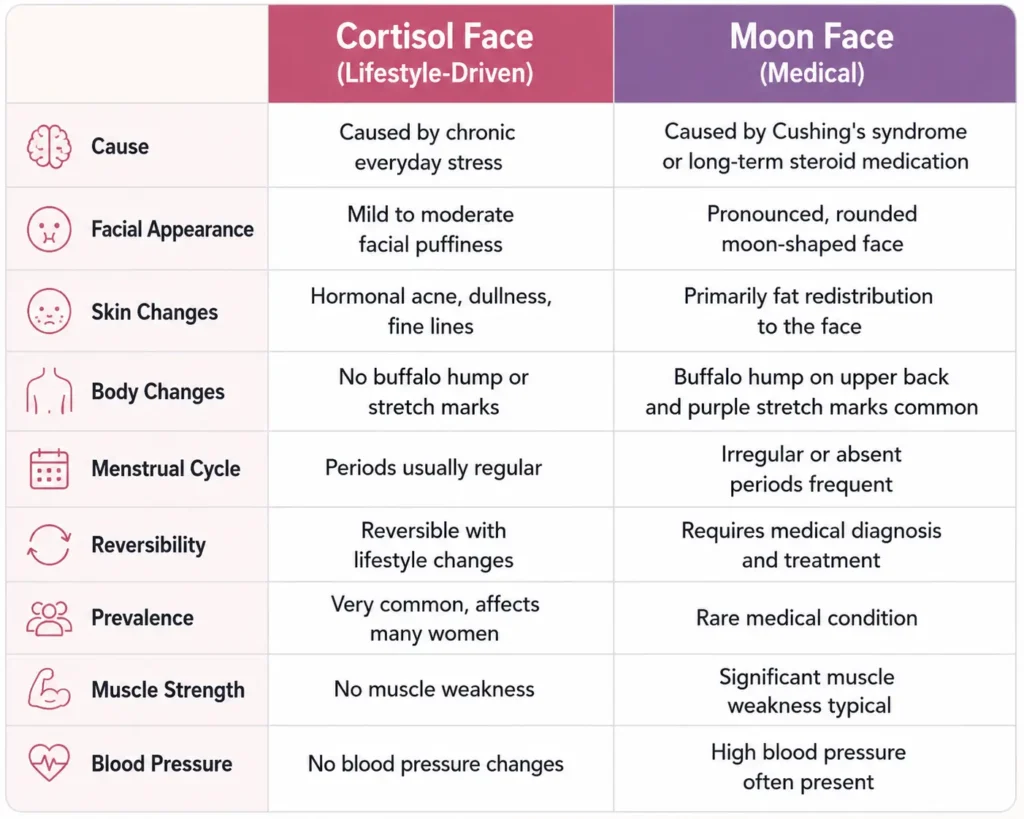
If your puffiness and facial changes are accompanied by the symptoms in the right column, that warrants a conversation with your doctor rather than a wellness routine. But for most women reading this, what you’re dealing with is stress-driven cortisol face, absolutely worth addressing, and very much within your control.
What’s Actually Causing High Cortisol Levels in Women?
Understanding your triggers is half the battle. The causes of chronically elevated cortisol in women are broader than most people realise. It’s not just about being stressed at work.
- Chronic psychological stress: prolonged emotional load, anxiety, relationship difficulties, financial pressure
- Poor or disrupted sleep: even one week of under-sleeping measurably raises cortisol levels the following day
- Blood sugar imbalances: skipping meals, high-sugar diets, and irregular eating patterns spike cortisol each time blood sugar crashes
- Over-exercising: particularly prolonged cardio or high-intensity training without adequate recovery
- Gut dysfunction: an unhealthy gut microbiome signals low-grade inflammation to the brain, which keeps cortisol elevated. This connection is explored in more depth in our guide on digestive health and the gut-hormone connection
- Perimenopause and menopause: declining oestrogen reduces the body’s ability to buffer cortisol, making stress responses more intense
- Caffeine overconsumption: multiple coffees a day, especially on an empty stomach, raise cortisol more than most women realise
- Scrolling and digital overstimulation: constant low-level information stress keeps the nervous system in a sustained alert state
What makes this particularly relevant for women is that our cortisol axis is more sensitive to certain triggers than men’s, particularly social stressors and disrupted sleep. We feel it faster, and we often carry the load longer before acknowledging it.
Common Cortisol Face Myths in Women (and What Science Says)
I have to address the myths here, because a lot of what circulates online about cortisol face is either incomplete or genuinely misleading.
Myth 1: It’s Just About Being Stressed
Stress is the trigger, but the mechanism is physiological. Cortisol face isn’t about feeling stressed. It’s about sustained hormonal dysregulation. You can feel calm and still have elevated cortisol if you’re sleeping poorly, skipping meals, over-exercising, or dealing with gut inflammation. Many women I’ve heard from were shocked to learn their supposedly healthy lifestyle habits were contributing to the problem.
Myth 2: Better Skincare Will Fix It
Skincare can support your skin’s recovery, but it cannot address the root cause. Applying a collagen serum while your cortisol is still elevated is like mopping the floor while the tap is still running. You need to address the hormone first, then support the skin topically. Products containing niacinamide, hyaluronic acid, ceramides, and azelaic acid are genuinely helpful adjuncts, but they’re secondary, not primary.
Myth 3: It Goes Away on Its Own When Things Calm Down
Sometimes, yes. But chronic cortisol elevation changes things structurally. Collagen doesn’t rebuild itself overnight, the HPA axis (the hormonal stress-response system) can take months to recalibrate after extended stress, and if poor habits have become entrenched, a calm period won’t automatically reset everything. Intentional recovery is required.
Myth 4: Only Highly Stressed Women Get Cortisol Face
Cortisol face doesn’t discriminate by visible stress levels. Some of the most zen-presenting women I’ve come across have been running on chronically elevated cortisol because of underlying gut issues, blood sugar dysregulation, or long-term sleep debt, none of which looks like classic stress from the outside. If the symptoms fit, they fit, regardless of how put-together your life appears.
How to Naturally Reverse Cortisol Face: A Realistic Timeline
Here is where I want to give you something genuinely useful, not a reduce-stress platitude, but a practical framework based on what actually moves the needle.
Step 1: Stabilise Blood Sugar (Week 1 to 2)
This is the most underrated cortisol fix. Every time your blood sugar crashes, your body releases cortisol to compensate. If you’re skipping breakfast, having coffee before food, or relying on refined carbohydrates, you’re triggering cortisol spikes multiple times a day without realising it.
Start eating within an hour of waking. Build every meal around protein, healthy fat, and fibre before adding carbohydrates. This single change has a measurable impact on cortisol levels within days for many women.
Step 2: Prioritise Deep Sleep (Week 1 to 4)
Cortisol and sleep have a bidirectional relationship. High cortisol disrupts sleep, and poor sleep raises cortisol. Breaking this cycle requires active sleep hygiene: consistent wake and sleep times, no screens for 60 minutes before bed, a cool dark room, and avoiding alcohol (which fragments sleep architecture even when it helps you fall asleep).
If you want to go deeper on this topic, our piece on the science behind stress and its long-term effects covers exactly how cortisol disrupts the nervous system and what to do about it.
Step 3: Move Differently (Week 2 to 6)
More intense exercise is not the answer here. If you’re already running on high cortisol, HIIT and long cardio sessions add to the hormonal load. Instead, prioritise walking, yoga, Pilates, and resistance training with adequate rest between sessions. A 30-minute walk in the morning is one of the most well-documented cortisol regulators. It lowers cortisol, improves insulin sensitivity, and exposes you to natural light, which helps reset your circadian rhythm.
Step 4: Use Adaptogens Strategically (Week 3 to 8)
Adaptogens are herbs that help modulate the HPA axis, the same system that drives cortisol dysregulation. The most well-researched for women include:
- Ashwagandha: shown in multiple studies to reduce cortisol levels significantly over 8 to 12 weeks
- Rhodiola rosea: particularly effective for stress-related fatigue and burnout
- Holy basil (tulsi): reduces cortisol, supports blood sugar balance, and has mild anti-inflammatory effects
- Reishi mushroom: a gentler option for nervous system support and immune regulation
These are not magic pills, and they work best as part of a broader protocol rather than in isolation.
Step 5: Feed Your Skin From the Inside (Week 2 Onwards)
Cortisol depletes key nutrients that your skin depends on, particularly vitamin C, zinc, magnesium, and omega-3 fatty acids. According to Healthline, foods that actively help lower cortisol include dark leafy greens, fatty fish, berries, avocado, dark chocolate (unsweetened), and fermented foods. Building your plate around these not only supports cortisol regulation but directly feeds collagen synthesis and skin repair.
What to Expect: A Realistic Timeline
- Week 1 to 2: Puffiness begins to reduce as blood sugar stabilises and inflammation settles
- Week 3 to 4: Skin tone starts to even out; breakout frequency decreases
- Week 6 to 8: Collagen synthesis begins improving; skin regains some luminosity
- Month 3 to 6: Structural skin improvements visible; fine lines less pronounced; overall skin health noticeably changed
This is a long game. Anyone promising a 2-week cortisol face fix is selling you something.
Skincare Routine for Cortisol Face: What Actually Helps
While you’re working on the internal root cause, a targeted skincare routine supports recovery and reduces the visible impact. Think of this as working alongside your lifestyle changes, not replacing them.
Morning: Gentle cleanser, then antioxidant vitamin C serum (rebuilds collagen, protects against stress-induced oxidative damage), then niacinamide (reduces redness, strengthens skin barrier, regulates oil), then SPF 50 (UV damage accelerates the collagen loss cortisol has already started).
Evening: Oil cleanser, then gentle exfoliant 2 to 3 times per week (lactic acid is ideal for stressed skin), then ceramide-rich moisturiser (repairs the disrupted skin barrier), then facial massage with a gua sha or jade roller (stimulates lymphatic drainage to reduce puffiness and promote circulation).
For hormonal acne specifically, azelaic acid at 10 to 15% is one of the most evidence-backed ingredients. It reduces inflammation, kills acne-causing bacteria, and fades post-inflammatory hyperpigmentation without the harshness of benzoyl peroxide.
If you’re navigating broader skin health concerns alongside cortisol face, our skin and beauty resource hub has deep-dive guides on everything from hormonal acne to barrier repair.
The Deeper Hormonal Picture: Why Women Are More Vulnerable
This is something rarely addressed in cortisol face content, and it matters.
Women’s hormonal systems are more sensitive to cortisol’s effects than men’s for several interconnected reasons. First, oestrogen plays a moderating role in cortisol regulation. It helps buffer the HPA axis response. When oestrogen fluctuates (during the luteal phase of your cycle, perimenopause, or postpartum), your sensitivity to cortisol spikes dramatically.
This is why many women notice their skin deteriorates most in the week before their period. Cortisol is higher, oestrogen is lower, and the combination is exactly the right environment for puffiness, breakouts, and dullness to peak simultaneously.
It’s also why cortisol face symptoms in women in their late thirties and forties are often attributed to ageing when what’s actually happening is a shifting hormonal landscape that makes the skin more cortisol-sensitive than it was before. Addressing hormonal balance holistically, not just stress in isolation, is often the missing piece. Our guide on natural hormone balance for women covers the full picture of what shifts as we age and what to do about it.
When Cortisol Face Symptoms Need Medical Attention
Most cases of cortisol face are stress and lifestyle-driven and respond well to the strategies above. But there are situations where you should see a doctor rather than trying to handle it yourself:
- Facial puffiness is accompanied by rapid unexplained weight gain, particularly in the abdomen and upper back
- You have pink or purple stretch marks appearing on the abdomen, thighs, or chest
- Your periods have become irregular or stopped
- You have unusual facial hair growth, particularly on the chin and upper lip
- Your skin is thinning and bruising easily without obvious cause
- You experience extreme fatigue, muscle weakness, or high blood pressure alongside facial changes
These can be signs of Cushing’s syndrome or another adrenal disorder that requires proper diagnosis and medical treatment. If this describes your situation, please seek a medical evaluation rather than relying on a wellness protocol.
Frequently Asked Questions About Cortisol Face
What does cortisol face actually look like?
Cortisol face typically presents as a combination of facial puffiness (especially in the morning), dull and tired-looking skin, hormonal acne along the jawline and chin, under-eye darkness or hollowing, and in some cases a slightly rounder facial shape due to fluid retention and fat redistribution. The key distinction is that these changes appear or worsen during high-stress periods and tend to affect multiple aspects of the skin simultaneously rather than in isolation. A single puffy morning after a late night is not cortisol face. It’s a pattern of symptoms that persists over weeks or months.
Is cortisol face the same as moon face?
No, and this distinction matters. Cortisol face is the general term for stress-driven skin and facial changes caused by chronically elevated lifestyle cortisol. Moon face is a specific medical term for the pronounced facial rounding associated with Cushing’s syndrome, a condition involving extremely high cortisol levels from a tumour or long-term corticosteroid medication use. Moon face comes with additional symptoms including a buffalo hump, severe muscle weakness, purple stretch marks, and irregular periods. If you have these alongside facial puffiness, see a doctor. If your symptoms are milder and stress-related, cortisol face is the more accurate description.
Can cortisol face be reversed naturally?
Yes, in most cases. Because lifestyle-driven cortisol face is caused by ongoing hormonal dysregulation, addressing the root causes (blood sugar stability, sleep quality, stress load, gut health, and movement) allows the body to recalibrate over time. Skin collagen rebuilds, inflammation reduces, and the visible symptoms gradually improve. The timeline is realistic rather than rapid: expect meaningful changes over 6 to 12 weeks with consistent effort, and more significant structural improvements over 3 to 6 months. Targeted skincare supports the process but works best in combination with internal changes rather than as a standalone fix.
How long does it take to reduce cortisol face?
The puffiness component, driven largely by fluid retention and inflammation, tends to respond fastest, often improving within 1 to 2 weeks of stabilising blood sugar and reducing the main stress triggers. Acne related to cortisol usually takes 3 to 6 weeks to noticeably decrease. Dullness and fine lines, which are driven by collagen loss, take longer, typically 2 to 4 months before you see meaningful skin texture improvements. The full reversal of structural changes can take up to 6 months. This is why it’s important to think of this as a lifestyle protocol rather than a short-term intervention
What foods help reduce cortisol face?
Several foods have documented effects on cortisol regulation. Foods rich in vitamin C (kiwi, bell peppers, citrus) support adrenal function and cortisol metabolism. Omega-3 fatty acids in salmon, sardines, walnuts, and chia seeds reduce the inflammation that cortisol drives. Magnesium-rich foods, dark leafy greens, pumpkin seeds, dark chocolate, help regulate the HPA axis and improve sleep quality. Fermented foods such as kefir, kimchi, and yoghurt support the gut microbiome, which communicates directly with the adrenal-cortisol system. Conversely, high-sugar foods, alcohol, and excessive caffeine all elevate cortisol, so reducing these has an immediate impact.
Does exercise make cortisol face worse?
It depends on the type and volume of exercise. High-intensity exercise and prolonged cardio (over 60 minutes) acutely elevate cortisol, which is fine in moderation but counterproductive when cortisol is already chronically high. For women dealing with cortisol face, the research supports shifting toward moderate-intensity exercise: walking, yoga, swimming, and resistance training with adequate recovery. These lower cortisol over time rather than adding to the hormonal burden. Morning walks in particular are well-documented for their cortisol-regulating effect, likely due to a combination of light exposure, gentle movement, and breathing pattern changes.
Can cortisol face cause permanent damage?
Long-term untreated cortisol elevation does cause structural changes to the skin, including collagen depletion, accelerated elastin breakdown, and thinning of the dermal layer, all of which take significant time and effort to reverse. However, the skin has remarkable regenerative capacity when given the right conditions. Even after years of chronic stress, meaningful skin recovery is possible with sustained lifestyle changes. The earlier you address it, the less structural damage accumulates, which is why recognising cortisol face symptoms in women early is genuinely valuable rather than cosmetic vanity.
What skincare ingredients help cortisol face?
The most evidence-backed ingredients for stress-related skin are: niacinamide (reduces inflammation, regulates sebum, strengthens the skin barrier), vitamin C serum (stimulates collagen synthesis and neutralises oxidative stress), ceramides (repairs the disrupted skin barrier common in cortisol face), azelaic acid (targets hormonal acne without stripping the skin), and hyaluronic acid (replenishes the hydration that cortisol-related barrier damage depletes). A gentle, non-stripping approach is key. Stressed skin does not tolerate harsh actives well. Avoid over-exfoliating or layering too many actives at once while the barrier is compromised
The Bottom Line on Cortisol Face
Your skin is not being dramatic. When cortisol face symptoms in women show up, the puffiness, the breakouts, the dullness, the lines that seem to appear overnight, it’s your body communicating something real about your internal hormonal state. The good news is that unlike ageing, which is irreversible, cortisol face is a condition you have genuine leverage over.
The approach that actually works isn’t complicated: stabilise blood sugar, protect sleep, move in ways that reduce rather than add to your stress load, support your gut, and feed your body the nutrients cortisol depletes. Add targeted skincare to support recovery, and give it real time. This is a 3 to 6 month commitment, not a quick fix.
If you’re ready to go deeper on the hormonal and stress side of this picture, explore our guides on hormonal balance for women and the science behind chronic stress. Understanding the full system is what makes the changes stick.
Medical Disclaimer:
This article is for informational purposes only and does not constitute medical advice. It is not a substitute for professional medical diagnosis or treatment. Consult a licensed dermatologist if you notice persistent or unusual nail changes.
About the Author
Syma Hussain | Women’s Health and Beauty Writer, wellInfinity.com
Syma Hussain is the founder and lead writer at WellInfinity, a holistic health platform empowering women through research-backed wellness advice. After years of navigating her own skin and nail health challenges, she turned her personal experience into a resource that cuts through generic advice and delivers what actually works.






